Sean Doerr Shares How He's Embracing Life with Pompe Disease
ASGCT Staff - February 06, 2020
In this Q&A, Sean Doerr, 29, talks about living his life with a genetic disorder that took years to diagnose, the importance of being your own advocate, and why he believes it's an "exciting time to have Pompe disease."

What was your life like before you were diagnosed with Pompe disease? When did you realize something was wrong, and how long did it take for you to receive your diagnosis?
Growing up, I honestly had no suspicion that anything was wrong with me, physically. Being that Pompe is a progressive disease, and having no metrics to compare of how your body should be physically, besides seeing major differences in others, made things tough. I think I was able to perform a single sit-up in my life, back when I was in high school. Personally, I thought the lack of core strength was just the result of being out of shape and never working out.
At the age of 12, I was diagnosed with type-1 diabetes. During my overnight stay at the hospital, blood work showed abnormally high liver enzymes. Long story short; a liver biopsy would later show results that were inconclusive. Around the age of 18, my dad had neurologist appointments after having Guillain-Barré syndrome and underlying muscle issues. The neurologist was intrigued by my father’s high CK [the enzyme creatine kinase] levels, and brought me in out of curiosity, testing both my CK and performing an EMG [Electromyography] (my father later tested as only a carrier of Pompe). Very high CK levels were found, and the EMG test results showed myopathy. I then had a muscle biopsy which was inconclusive in findings. For the years after, I was seen by a half-dozen different neurologists and gastroenterologists which were unable to determine what caused the muscle damage and abnormal blood work.
With the technology of genome sequencing I knew the very mutations that were responsible for the Pompe disease.
Sean Doerr
By 2018, I was convinced I had a rare disease that would likely never see a diagnosis. Luckily the endocrinologist I saw for my diabetes always had an inclination to explore my other ailments, frequently performing blood work to track my liver and muscle functions. At her urging, I booked an appointment with a neurologist she recommended. After a quick site visit, and an EMG visit, I was given a lab order that tests for acid maltase levels in the blood. As someone who researches any lab tests or results out of pure curiosity and the quest for knowledge, I quickly came upon Pompe disease. Some symptoms of the disease I had, while other, more severe symptoms, did not affect me. The test result came back with low levels of the enzyme tested, indicative of Pompe. From there, I had the final conclusive test of genome sequencing. In a matter of a few weeks, I was given the diagnosis which would be indisputable. With the technology of genome sequencing I knew the very mutations that were responsible for the Pompe disease, and with the two pathogenic variants of the GAA enzyme expressed at a dozen or so characters each (c.-32-13T>G and c.1655T>C to be exact), the severity of the disease can be compared with other patients to track and predict progression. As a friend with Pompe in California always says, Pompe… it’s in my DNA!
How did your diagnosis change your day-to-day activities? What treatment options were available when you were diagnosed?
Day-to-day living with Pompe disease is a challenge, it could always be much easier and could also be much more difficult. Around the time of diagnosis, I did notice that my breathing had begun to decline, and things like stairs and bending over to pick something off the floor were getting harder.
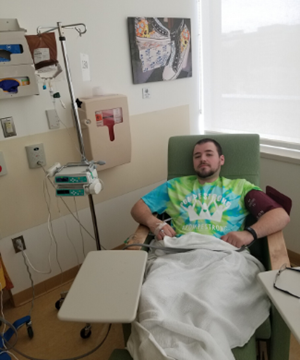 Treatment-wise, the only approved therapy is an enzyme replacement that takes place biweekly for the rest of my life. While the infusion typically takes about 3-4 hours, it also involves over an hour to mix the drug for an adult. For my treatment, it takes a nurse or pharmacist mixing saline with over 39 vials (it’s all weight based). While most patients have no problem on this treatment, my body fought it hard; I experienced allergic reactions and high sustained antibodies. Initially I had a home nurse giving my infusion to me in the morning, soon after my 12-hour midnights shift, where I planned to sleep the entire time (the goal was to enjoy my free and awake time not strapped down to an IV). Soon after I started my infusions, I would awake to rigors, some so bad that talking was difficult. I was forced to go to an infusion center, have my infusion rate slowed down (it’s about 5 hours long at this point), and undergo immunosuppression, which is still underway, and will likely have to be repeated (the protocol lasts about 6 months and my antibody levels are not low enough to an acceptable level). The immunosuppression makes for four additional drugs and a lot more days of infusion, with as many as 3 visits to the infusion center in a 5 day period. It makes for a busy schedule.
Treatment-wise, the only approved therapy is an enzyme replacement that takes place biweekly for the rest of my life. While the infusion typically takes about 3-4 hours, it also involves over an hour to mix the drug for an adult. For my treatment, it takes a nurse or pharmacist mixing saline with over 39 vials (it’s all weight based). While most patients have no problem on this treatment, my body fought it hard; I experienced allergic reactions and high sustained antibodies. Initially I had a home nurse giving my infusion to me in the morning, soon after my 12-hour midnights shift, where I planned to sleep the entire time (the goal was to enjoy my free and awake time not strapped down to an IV). Soon after I started my infusions, I would awake to rigors, some so bad that talking was difficult. I was forced to go to an infusion center, have my infusion rate slowed down (it’s about 5 hours long at this point), and undergo immunosuppression, which is still underway, and will likely have to be repeated (the protocol lasts about 6 months and my antibody levels are not low enough to an acceptable level). The immunosuppression makes for four additional drugs and a lot more days of infusion, with as many as 3 visits to the infusion center in a 5 day period. It makes for a busy schedule.
Lastly, every year, in addition to seeing my geneticist biweekly, I have to visit many specialists, since the disease affects so many muscle groups. June of every year is jammed packed with visits to a pulmonologist, physical therapist, cardiologist, and neurologist. I had to get off my HMO insurance, as getting referrals from a primary care doctor was a major inconvenience.
At what point did you get involved in advocacy work? What type of work are you involved in now, and why do you think it’s so important to get (and stay) involved in advocacy?
As a patient with Pompe disease, I would say, without a doubt, you have to be an advocate. Imagine going to a specialist for the first time, the doctor asks you the reason for the visit, and gives you a blank stare when you say Pompe disease. Having the rare disease that is Pompe, the fact that I possess a unique disorder that most have no idea of, is a story that needs to be told and shared with anyone that is interested. From an advocacy perspective, the knowledge of Pompe, the future of treatments of Pompe, the diagnostic tools of Pompe, they all need to be shared and encouraged. To be able to share my story and of what Pompe is, is the ability to educate and inform.
It’s odd to explain, but I’ve never felt so in control of a disease, in the sense that I know my contributions can and will have a direct impact on the future of the disease.
Sean Doerr
Right now there are about a half-dozen companies developing treatments for the disease. If others with Pompe do not advocate, nor take part in clinical trials, the chance that better treatments and therapies will make it to release are threatened. For a common disease, studies and trails can find many candidates to advance treatment, while rare diseases have a small population that is able to commit and complete crucial studies. It’s odd to explain, but I’ve never felt so in control of a disease, in the sense that I know my contributions can and will have a direct impact on the future of the disease. It’s a completely different feeling with Pompe as opposed to diabetes, where I feel the idea of a cure or innovations seem unlikely, the story has been told, and there are many taking charge in advocacy.
 As soon I as I received my diagnosis, I jumped right into advocacy. I called to setup screening for a clinical trial the same day I received official word I had Pompe. In just under two short years, I am humbled to be a part of four patient advocacy boards (three drug companies and one non-profit), spoke to the press and launched MDA’s Fill-The-Boot campaign for my employer/fire department, spoke to my congress members on Capitol Hill during Rare Disease Week, and shared my story on Intentional Pompe Day (April 15) to its official blog.
As soon I as I received my diagnosis, I jumped right into advocacy. I called to setup screening for a clinical trial the same day I received official word I had Pompe. In just under two short years, I am humbled to be a part of four patient advocacy boards (three drug companies and one non-profit), spoke to the press and launched MDA’s Fill-The-Boot campaign for my employer/fire department, spoke to my congress members on Capitol Hill during Rare Disease Week, and shared my story on Intentional Pompe Day (April 15) to its official blog.
I also share my story with a Facebook page and Instagram, called PompeTrek. I bought a former ambulance on the week of my first enzyme replacement therapy. I’m slowly building it into one awesome motorhome, because life is what you make it, and Pompe will not stop me from seeing the world and sharing my story.
For someone who is living their life with a genetic disease, what would you tell them? How can they get involved in working toward a treatment?
 I always say you have to be your own advocate. No matter what you have, it is a part of you, your story, and you can wear it with pride, or treat it as something you hide and are ashamed of. Everyone’s circumstance is different, but if you can turn something negative into a positive, I think the choice is obvious. Seek and find others like you. My journey with Pompe was made so much easier when I found of Facebook groups, non-profits dedicated to the disease, and patient meetings.
I always say you have to be your own advocate. No matter what you have, it is a part of you, your story, and you can wear it with pride, or treat it as something you hide and are ashamed of. Everyone’s circumstance is different, but if you can turn something negative into a positive, I think the choice is obvious. Seek and find others like you. My journey with Pompe was made so much easier when I found of Facebook groups, non-profits dedicated to the disease, and patient meetings.
When it comes to getting involved toward treatment, I have found that monitoring clinicaltrials.gov is one of the best places to find how you can have a direct impact in changing the future. Clinical trials are not for everyone, but every bit helps, and you should consider what your participation will do to benefit yourself and your disease community as a whole.
Having an ailment or disease is of course with its downfalls, as I don’t think anyone, myself included, would turn away a cure, and the chance to cease the impairment we had forced upon us. Having a good friend, doctor, therapist to open up, share experiences, opinions, happiness, and grievances is very important. Perhaps one of the best parts of being active in advocacy is when I can share a drink with a fellow patient who I met for the first time. It’s something magical when you can connect on a deep level to someone who has gone through much of the same journey and experienced the same hardships. I’ve formed deep friendships with many people from across the world, despite only knowing them in person for a few short hours.
What does your life look like now? What are your hopes for the future of Pompe treatment?
I’m living life to the fullest. I live my life the best I can around Pompe and treatments. The scariest part of the disease is not knowing just how I will how progress, and when. Due this fact, I will continue to be as active I can in advocacy and will seek out opportunity in travel and activities that I can do now while in my best physical shape. In 2019, I went through a firefighter academy, to put in perspective the reality of my life with Pompe. Physically it was difficult, even mentally difficult at times. It is an accomplishment I am proud of. It also put helped me see the unfortunate reality that I am deficient in many ways that I did not know, or previously underestimated. Presently, I am attending graduate school to pursue a master’s in public administration.

Fortunately, the future of Pompe is very promising. The current enzyme replacement therapy was seen as a major breakthrough a decade ago. I am confident that within this decade the next generation of therapy will arrive—gene therapy. Many companies are rushing to develop gene therapy to produce the enzyme I am deficient in, with one clinical trial already underway and dosing patients. Rather than spending an entire day strapped to an IV that feeds me the GAA enzyme, someday I will continuously produce the enzyme internally, introduced by gene therapy. What an exciting time to have Pompe disease.
To learn more about Pompe, check out our Patient Education resources.
Related Articles
Maria Santaella, PhD (c), MSN, RN-BC, CPHON serves as the Vice President of Research for the National Bleeding Disorders Foundation. During the workshop she spoke on clinical trial enrollment by sharing strategies to address barriers in recruiting.
Annual Meeting 2024
Inclusive Trial Design Amplifies Patient Voices and Drives Meaningful Outcomes
Samuel Hughes, MBA, St. Jude Children's Research Hospital - June 18, 2024
Patient Perspectives
Rare Village Foundation Lets Rare Disease Families Know They're Not Alone
Devin Rose - October 05, 2023
Patient Perspectives
From Camp to Capitol Hill, Jordan Howard Advocates for Hemophilia
Devin Rose - April 17, 2023
Patient Perspectives
Through the Pain of Fabry Disease, Artist Wes Burian Hasn’t Let Go of Hope
Devin Rose - February 28, 2023